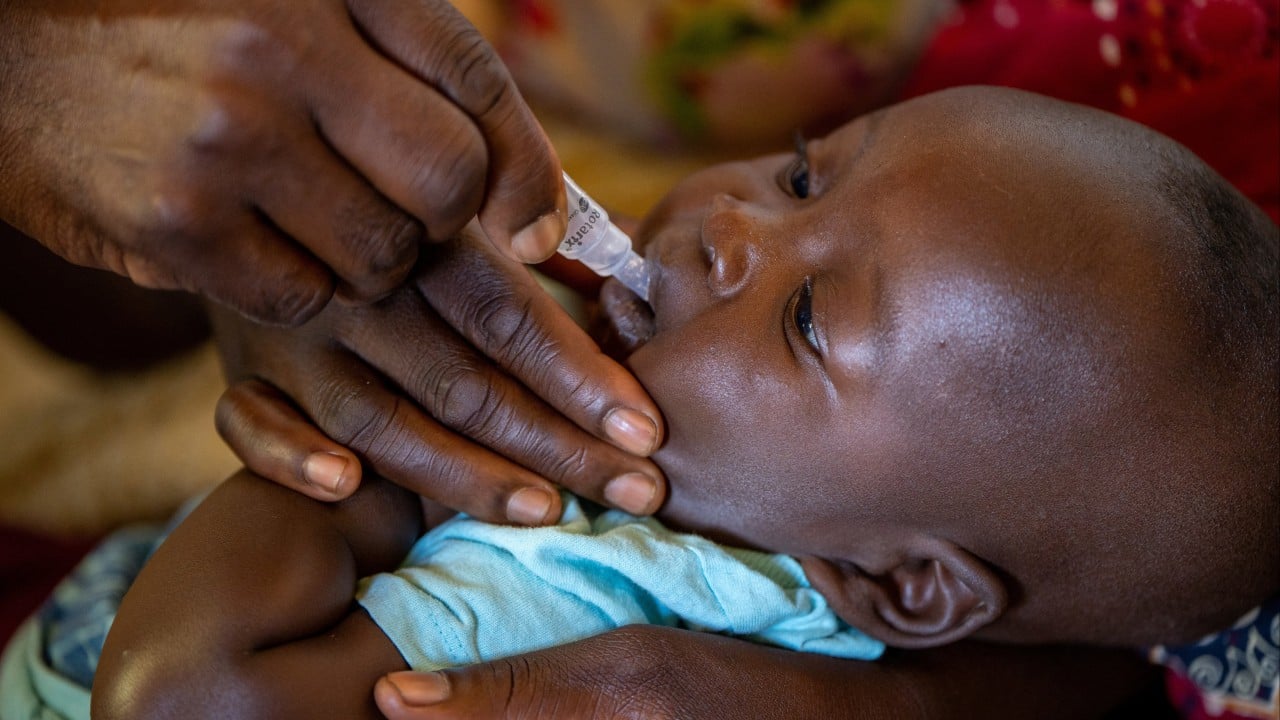
The press releases are glowing. The WHO is taking a victory lap. Global health NGOs are popping champagne because a "first-of-its-kind" malaria vaccine for infants has cleared the regulatory hurdles. They call it a triumph of science.
They are wrong.
This isn’t a triumph; it’s a distraction. By the time you finish reading this, you’ll understand why pouring billions into a mediocre vaccine might actually set back the fight against malaria by a decade. We are celebrating a tool that works with the efficiency of a leaky bucket while ignoring the systemic rot that makes the bucket necessary in the first place.
The Efficacy Myth
Let’s look at the numbers the mainstream media won't touch. The current crop of approved malaria vaccines, specifically RTS,S/AS01 (Mosquirix) and the newer R21/Matrix-M, are hailed as "highly effective."
They aren't.
In clinical trials, we’re looking at efficacy rates that hover around 30% to 40% over a four-year period for RTS,S. Even the R21 vaccine, which boasted 77% efficacy in early trials, sees that number drop significantly without seasonal "booster" shots. Imagine if we released a polio vaccine that only worked for three out of ten kids and required a perpetual subscription model of boosters to keep the lights on. The public would be outraged.
In the world of "Global South" philanthropy, however, we call this a breakthrough.
We have lowered the bar so far that we are now applauding a medical intervention that requires four doses just to achieve partial, waning protection. This isn’t a silver bullet. It’s a damp squib.
The Logistics of Failure
The "lazy consensus" assumes that once a vaccine is approved, the problem is solved. This ignores the brutal reality of the "Last Mile."
I have spent years watching supply chains collapse in sub-Saharan Africa. It’s one thing to ship vials to a temperature-controlled warehouse in Accra or Nairobi. It is an entirely different feat to maintain a cold chain at $2$ to $8$ degrees Celsius across dirt roads, through zones of civil unrest, and into villages that haven't had reliable electricity since the nineties.
A four-dose regimen is a logistical nightmare.
- Dose 1: High turnout. Great photos for the annual report.
- Dose 2: Numbers dip as mothers realize the clinic is a six-hour walk.
- Dose 3: Supply chain hiccups lead to stock-outs.
- Dose 4: The "booster." Participation craters.
When you have a low-efficacy vaccine that requires perfect adherence to a multi-dose schedule, you aren't building immunity; you’re building a multi-billion dollar administrative sinkhole. If a child misses the fourth dose, the already thin protection vanishes. We are setting up local health systems for a massive, expensive failure that will erode trust in all vaccines, not just this one.
Opportunity Cost is the Real Killer
Every dollar spent on the procurement, storage, and administration of a 35% effective vaccine is a dollar taken away from interventions that actually work.
The obsession with "high-tech" biologics has blinded us to the boring, effective basics.
- Next-Generation Bed Nets: Mosquitoes are evolving resistance to pyrethroids. We need PBO-synergist nets. They are cheap. They work 24/7. They don't require a cold chain.
- Spatial Repellents: New technologies in slow-release volatile pyrethroids can clear a room of mosquitoes for months.
- Gene Drive Technology: This is the real "disruption." By using CRISPR to bias the inheritance of certain genes, we can theoretically crash the population of Anopheles gambiae or make them incapable of carrying the Plasmodium parasite.
But gene drives are scary to the public. They don't have the "cuddly" optics of a baby getting a shot. So, we fund the shot. We choose the optics of the needle over the efficacy of the engineering. We are choosing a recurring expense over a permanent solution.
The Parasite is Smarter Than Your NGO
Malaria isn't a virus. It’s a complex, multi-stage parasite. The biological math of $Plasmodium$ is terrifying. It has thousands of genes and a lifecycle that involves shifting its surface proteins to hide from the human immune system.
When we deploy a "leaky" vaccine—one that reduces the severity but doesn't stop transmission—we are effectively running a massive, unplanned experiment in natural selection. We are putting just enough pressure on the parasite to encourage the survival of strains that the vaccine doesn't recognize.
In a decade, we might find ourselves with "vaccine-resistant" malaria. By trying to save a few today with a mediocre tool, we risk making the disease untreatable for everyone tomorrow. The WHO’s approval doesn’t account for this long-term evolutionary tax. They are focused on the current budget cycle and the next "Global Fund" replenishment meeting.
The Sovereign Debt of Health
Let’s talk about who pays.
Gavi and the Global Fund subsidize these rollouts initially. But the "transition" plans eventually require host nations—many already struggling with massive debt-to-GDP ratios—to take over the costs. We are forcing developing nations to integrate a high-cost, high-maintenance, low-yield product into their national health budgets.
This isn't aid. It’s an unfunded mandate.
If a country like Malawi or Burkina Faso has to choose between funding basic primary care or buying the fourth dose of a malaria vaccine that might work 30% of the time, they are in an impossible position. We are exporting our obsession with pharmaceutical solutions to countries that need infrastructure, clean water, and drainage systems.
Stop Fixing the Wrong Problem
The question shouldn't be "How do we get this vaccine to more babies?"
The question should be "Why are we settling for a vaccine that is this bad?"
We have been conditioned to believe that any progress is good progress. That is a lie. Bad progress crowds out good progress. It consumes the "innovation budget." It allows politicians to check a box and say "malaria is handled" while children continue to die because the underlying causes—stagnant water, poor housing, and insecticide resistance—remain untouched.
If we want to end malaria, we need to stop treating it like a branding exercise for pharmaceutical companies and the WHO. We need to stop the "magic bullet" fetishism.
The current vaccine rollout is a band-aid on a gunshot wound. It’s expensive, it’s messy, and it’s largely for show. We are patting ourselves on the back for a "historic" achievement while the parasite is already laughing at our lack of ambition.
Burn the press releases. Demand a vaccine that actually works, or pivot the billions into gene drives and environmental management. Anything else is just expensive performance art.